Communicable Disease Surveillance Highlights report on data
from various sources, including the National Notifiable Diseases Surveillance
System (NNDSS) and several disease specific surveillance systems that provide
regular reports to Communicable Diseases Intelligence. These national data
collections are complemented by intelligence provided by State and Territory
communicable disease epidemiologists and/or data managers. This additional
information has enabled the reporting of more informative highlights each
quarter.
The NNDSS is conducted under the auspices of the Communicable
Diseases Network Australia.
NNDSS collates data on notifiable communicable diseases from State or Territory
health departments. The Virology and Serology Laboratory Reporting Scheme
(LabVISE) is a sentinel surveillance scheme which collates information on
laboratory diagnosis of communicable diseases. In this report, data from
the NNDSS are referred to as ‘notifications’ or ‘cases’, and those from ASPREN
are referred to as ‘consultations’ or ‘encounters’ while data from the LabVISE
scheme are referred to as ‘laboratory reports’.
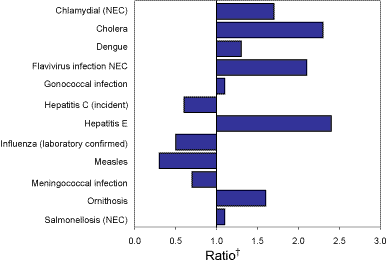
Figure 1 shows the changes in disease notifications with an onset in third quarter 2004 compared with a 5-year mean for the same period. The number of notifications received in the quarter was above the five year mean for chlamydial infections, cholera, dengue, flavivirus (NEC), gonococcal infections,
hepatitis E and ornithosis. The number of notifications received was below
the five year mean for hepatitis C (incident), influenza, measles, and meningococcal
disease.
Figure 1. Selected* diseases from the National Notifiable Diseases Surveillance System, comparison of provisional totals for the period 1 July to 30 September 2004 with historical data*
 Top of page
Top of page
Gastrointestinal diseases
Hepatitis A
There was a small cluster of five cases of hepatitis A infection in children
at a New South Wales primary school
in July. One of the cases was a sibling of one of the students. Immunoglobulin
prophylaxis was given to students and no further cases were reported. The
source of the infection appears to be a confectionary jar.
Later in July, patrons of a city caf� in Sydney were contacted to receive hepatitis A immunoglobulin therapy
after a caf� employee was diagnosed with hepatitis A. more than 100 people
received the prophylaxis and there were no cases reported.
Despite these cases, the number of notifications in the third quarter
(n=73) was well below the five year mean for the quarter (172).
Listeriosis
There were 16 cases of listeriosis reported in the third quarter. These
occurred in all states except the Northern Territory
and Tasmania (Table 2). Most cases
occurred in the elderly (median age 68.5 years).
Two maternal foetal cases of listeriosis were reported at a maternity
unit in Victoria. The first baby
was very ill and died shortly after birth. Listeria monocytogenes
was cultured from the placenta and blood culture. A second baby born 27 hours
later was well at birth and Listeria was cultured
only from placenta swabs, while blood cultures were negative. The mother
of the second baby had negative cultures of urine and high vaginal swabs.
Examination of the Listeria isolates indicated that
they were the same strain. It was concluded that the placenta of the second
baby was contaminated during examination in the delivery suite or in the
laboratory and that the second case was not a maternal foetal pair.
Quarantinable diseases
Cholera
Three cases of cholera were reported in the third quarter, one from New South Wales and the other from Victoria. One was a Vibrio cholerae 01 El
Tor infection and the other two were both Vibrio cholerae
01 Ogawa. All three infections were acquired overseas.
Top of page
Vaccine preventable disease
Measles
There were 12 cases of measles reported in the third quarter. Notifications
were received from New South Wales (2), South
Australia (3), Victoria (5) and Western
Australia (2). This total is well below the 26 cases reported in the same
period last year and the average of 24 cases reported in the period over
the past five years.
The reported measles infections were acquired in seven overseas travellers
and their contacts and of the remaining five cases, two were an unvaccinated
child and its mother; one was a sporadic case in an unvaccinated 21 year-old
and the other two cases were partially vaccinated children under two years
of age (NSW).
Influenza
There was a total of 1,082 notifications of laboratory confirmed influenza
in the third quarter, which was well below the three year mean for this period
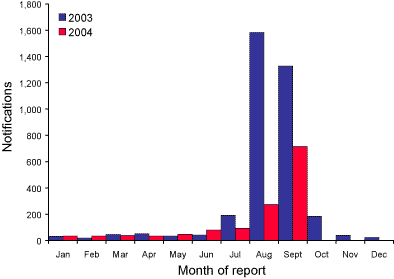
(2,233 notifications). In contrast to 2003, the peak in influenza activity
appeared later in the year and at a lower level (Figure 2).
Figure 2. Notifications of laboratory confirmed influenza, Australia 2003 and 2004 (to end September)
Two outbreaks of influenza-like illness were reported in army barracks,
during the quarter. The first in Victoria
occurred in new recruits, with a total of 94 cases, eight of which were typed
as A/Fujian (H3N2)-like. Although vaccination is not compulsory, influenza
vaccine is offered to all new recruits with an uptake rate of 73%. The second
outbreak of influenza-like illness occurred during a military exercise in Queensland involving military personnel from around
the country.
Top of page
In September, 13 outbreaks of influenza-like illness were reported from
residential institutions in NSW, including 12 aged care facilities (ACFs)
and one correctional centre. The outbreaks had high attack rates (up to 76%
of residents and 42% of staff) and death rates of up to 20% in residents.
In response to these outbreaks, public health unit staff provided advice
to facility managers on control measures. NSW Health developed guidelines
to assist ACF managers to minimise the spread of influenza within their institutions.
The guidelines document Controlling influenza outbreaks in aged care facilities
http://www.health.nsw.gov.au/living/flucontrol_cdfs.html was distributed to ACFs throughout New South Wales.
In previous years, NSW Health has not actively solicited reports of influenza
outbreaks from institutions, or systematically collated information on reported
outbreaks. The reasons for the apparent large number (13) reported in NSW
in September 2004, and the large proportion of these reported from the Hunter
Area, are unclear. One explanation could be improved reporting in 2004 following
the release of the Controlling Influenza Outbreaks in Aged Care
Facilities guidelines. The first outbreak was associated with
substantial media interest that may in turn have led to improved reporting
by other ACFs.
NSW Health provides Australian Government-funded influenza vaccine annually
to residents of ACFs. However, in the investigation of these outbreaks, public
health units found that residents' immunisation records did not provide clear
evidence of vaccination, perhaps because the turnover of residents in ACFs
was sometimes high and the immunisation status of new residents was not always
assessed on admission.
Annual immunisation of both residents and staff before winter (when the
influenza activity usually begins) is essential to limit the extent of such
outbreaks. ACF managers should ensure that record systems are in place to
document the vaccination status of residents and staff, and flag the records
of new residents and staff to ensure that they are offered immunisation.
With growing evidence that anti-influenza medicines are effective in slowing
outbreaks, ACF managers and clinicians should strongly consider their use
to limit the spread of the infection in residential facilities
(A full report is available at:
http://www.health.nsw.gov.au/living/infectreport.html)
Pertussis
There were 2,588 notifications of pertussis in the third quarter. One
thousand and ninety-seven were from New South Wales
and 779 were from Western Australia. Western
Australia had the highest rate (159.6 cases per 100,000 population, Table
3).
An increase in notifications of pertussis in Western Australia has been noted since May. Increased notification
rates were first observed in the Great Southern region around Albany
and Denmark in May, and
subsequently in the Goldfields, South-West, Wheatbelt and metropolitan Perth
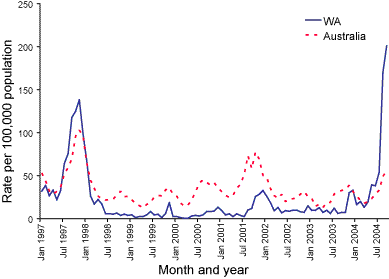
regions. Notifications are at the highest level recorded in the State since
1997(Figure 3). A relatively high proportion of notifications have been in
secondary school aged children (25%) and adults (38% in those aged 25 years
and above), compared to primary school aged students (18%) and younger children
(12%). Given evidence that secondary school aged students have been pivotal
in propagating transmission, a mass vaccination campaign in WA secondary
schools using dTpa (Boostrix TM) vaccine was implemented in the 4th school
term, in an attempt to limit the extent of the epidemic.
Figure 3. Notification rates of pertussis, Western Australia and Australia 1997 to September 2004 (per 100,000 population)
Top of page
Other bacterial infections
Meningococcal infections
There were 125 notifications of meningococcal infection in Australia in the third quarter.
This number is well below the average number of notifications for this period
received over the past five years (229 notifications).
There was serogroup data available on 89 of the notified cases in the
quarter. Fifty seven (64%) were serogroup B, 26 were serogroups C (29%),
five were serogroups W135 and there was a single case of serogroup Y.
A community based outbreak of meningococcal group C involving a rural
High School in the North East of Tasmania occurred between 26 July, 2004
and 9 August, 2004. The total number of cases involved in this outbreak was
four, all of which were later diagnosed as group C meningococcal infection.
Of the four cases, three were fourteen year old students at the High School.
The strain that caused the outbreak was later identified as C;P1.7-2.4. During
the course of the outbreak, staff from the PEHS Hobart office provided antibiotic
clearance to 87% of the students at the High School, and in association with
the local Council, assisted in the delivery of meningococcal C conjugate
vaccine to 84% of the students at the school. This increased coverage for
meningococcal C vaccine in the High School to 95%.
A national immunisation program began in New Zealand during the quarter
against the meningococcal serogroup B subtype B4P1.4/1.4(7), which has been
responsible for a 14-year epidemic in that country. A review of meningococcal
serogroup data in Australia (1995–2003) collected through the National Neisseria
Network was conducted by the National Centre for Immunisation Research and
Surveillance (NCIRS) to determine trends in the prevalence of the ‘New Zealand’
strain in Australia. The review found that despite over all increases in
the incidence of meningococcal disease in Australia, the overall incidence
of the New Zealand strain remained low (0.17 per 100,000 population). There
was an overall increase in the number of isolates of the New Zealand stain
detected in the period 1999–2003 (n=165) compared with the period 1995 to
1998 (n=56) with most this increase seen in New South Wales and Victoria
(Puech and McIntyre, 2004 unpublished).
Other diseases
M. ulcerans
There was an outbreak of Mycobacterium ulcerans
infections at Point Lonsdale in Victoria and two cases reported in Darwin
in the Northern Territory during the quarter. M. ulcerans
infections have been recognised in two geographic foci in Australia—one in
the Gippsland region of Victoria and the second in the Daintree region of
Queensland. The current outbreak which involved 14 people, appears to be
a new endemic focus. There is no information as yet as to whether there is
a focus in the Northern Territory.
With thanks to: Mark Bartlett (NSW Health),
Lynne Brown (DHS, Victoria), David Coleman and Avner Misrachi (DHHS, Tasmania).
This report was published in Communicable Diseases Intelligence Vol 28 No 4, December 2004.
